
Implant-free Rhinoplasty
A natural-looking nose without the use of artificial implants
This procedure creates a three-dimensional and natural-looking nasal contour using the patient’s own tissue, without inserting any artificial implants.
It is especially suitable for patients who prefer not to use artificial implants or for those who already have sufficient and high nasal bridge and therefore do not require an implant. In such cases, non-implant rhinoplasty can be an ideal option.
The procedure is customized based on the individual nasal structure and skin characteristics, helping to avoid potential side effects
associated with artificial implants. As a result, the nose is refined into a natural and aesthetically pleasing shape that closely
resembles the patient’s original anatomy.
Use of Autologous or Donor Dermis and Cartilage
Since each type of autologous tissue has its own characteristics, advantages, and limitations, it is essential to carefully select the most appropriate tissue based on the patient’s individual condition and needs.
Choosing the optimal tissue plays a crucial role in achieving safe and effective surgical outcomes.
Autologous Dermis
With the use of patient’s own
dermal tissue, this has a low
risk of side effects and
provides a natural texture.
Fascia
Harvested from the deep
temporal area inside the scalp,
fascia is mainly used in revision
surgeries or in patients with thin
scalp.
Rib cartilage
It has minimal risk of side
effects and provides strong
structural support and
durability.
Ear Cartilage
It has elastic and flexible nature
and is used to reinforce areas
where nasal cartilage is
insufficient.
Septal Cartilage
It is harvested inside the
nose to extend the nose tip
and nasal bridge
This procedure enhances the nasal bridge and tip using autologous tissues—such as ear cartilage, septal cartilage, and rib cartilage
without the use of artificial implants.
1. When Using Ear Cartilage
It is a surgical method that improves overall height and tip of the nose by correcting the nasal column, bridge and tip of the nose using
ear cartilage only.
Harvesting Ear Cartilage
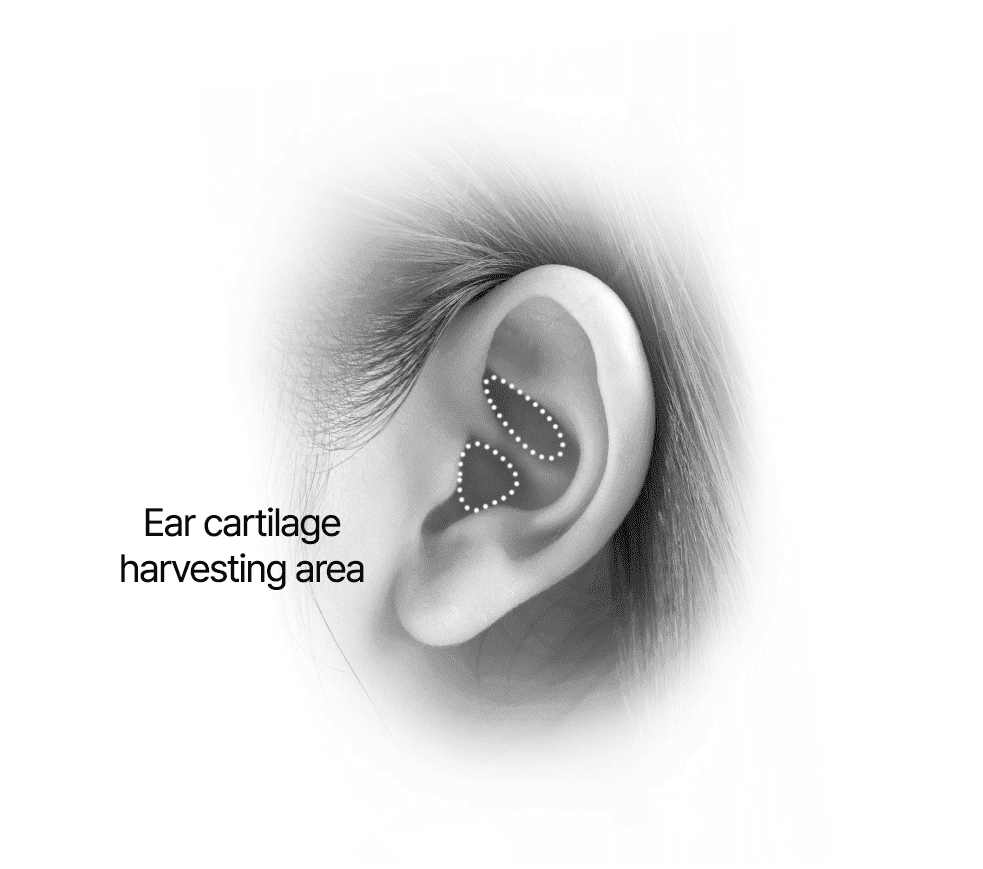
Nasal Bridge, Columella and Tip Correction Using Ear Cartilage
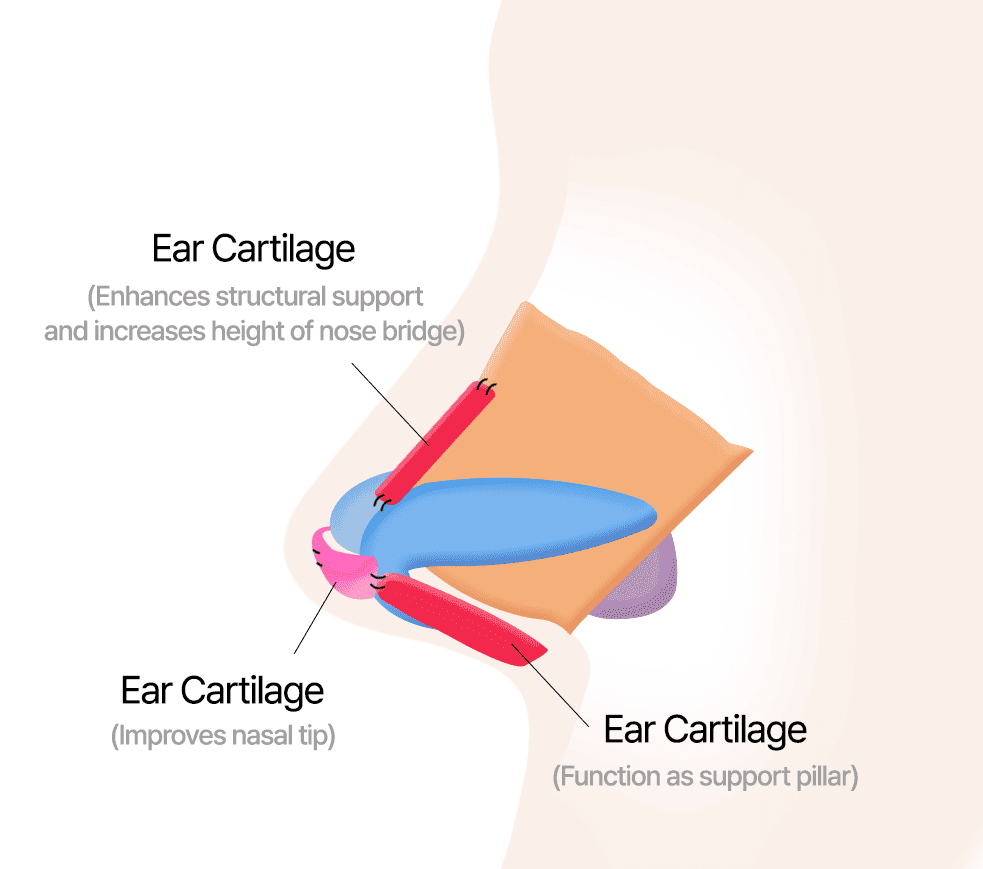
2. When Using Ear Cartilage and Septal Cartilage
This is a surgical procedure which takes advantage of both ear and septal cartilage. Ear cartilage is used in areas where
curvature is required while septal cartilage is applied to areas that need stronger structural support and straightness.
Harvesting ear and septal cartilages
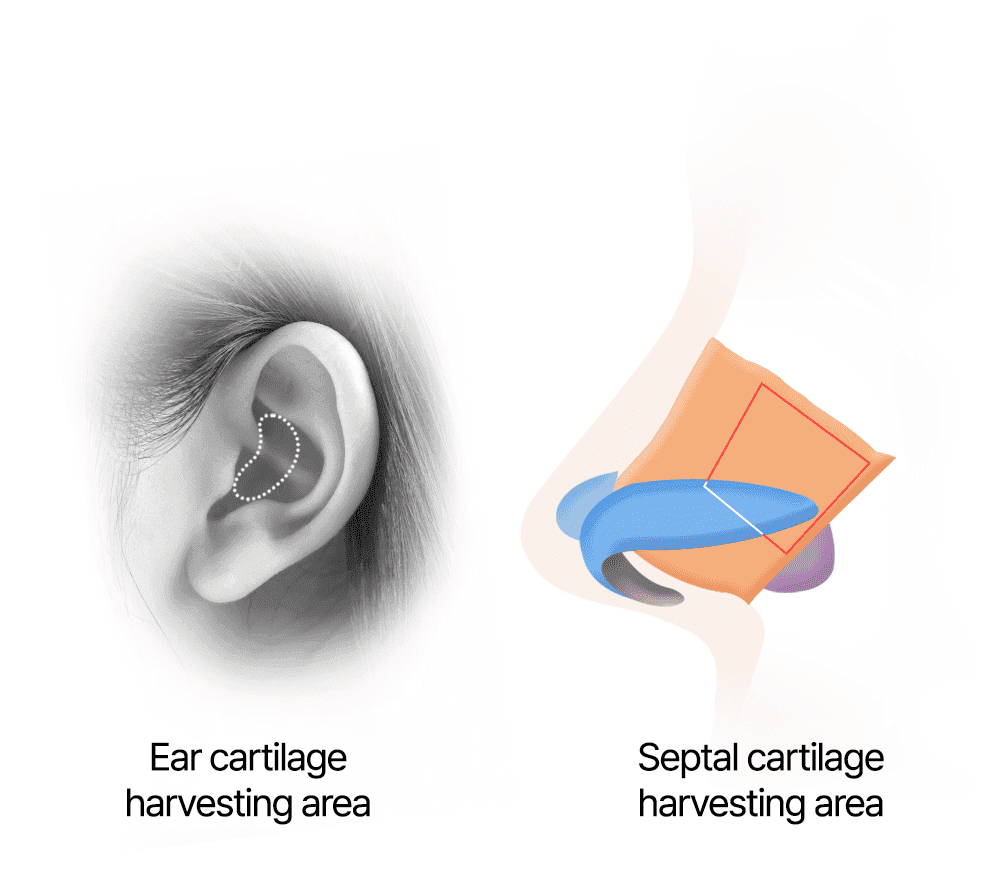
Correction utilizing ear and septal cartilages
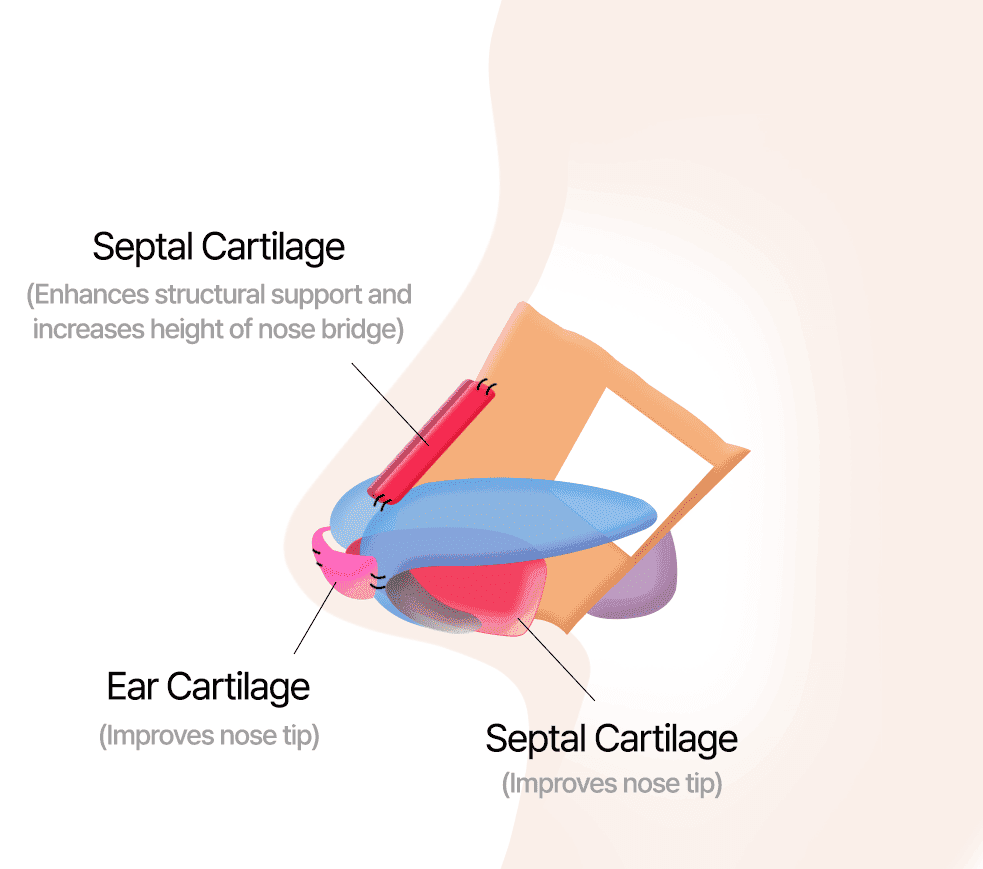
3. When Using Rib Cartilage
Rib cartilage is an autologous tissue with strong structural support which is suitable for short nose correction, revision cases
for contracted nose and primary rhinoplasty in patients who desire significant changes to nasal bridge.
Harvesting Rib Cartilage
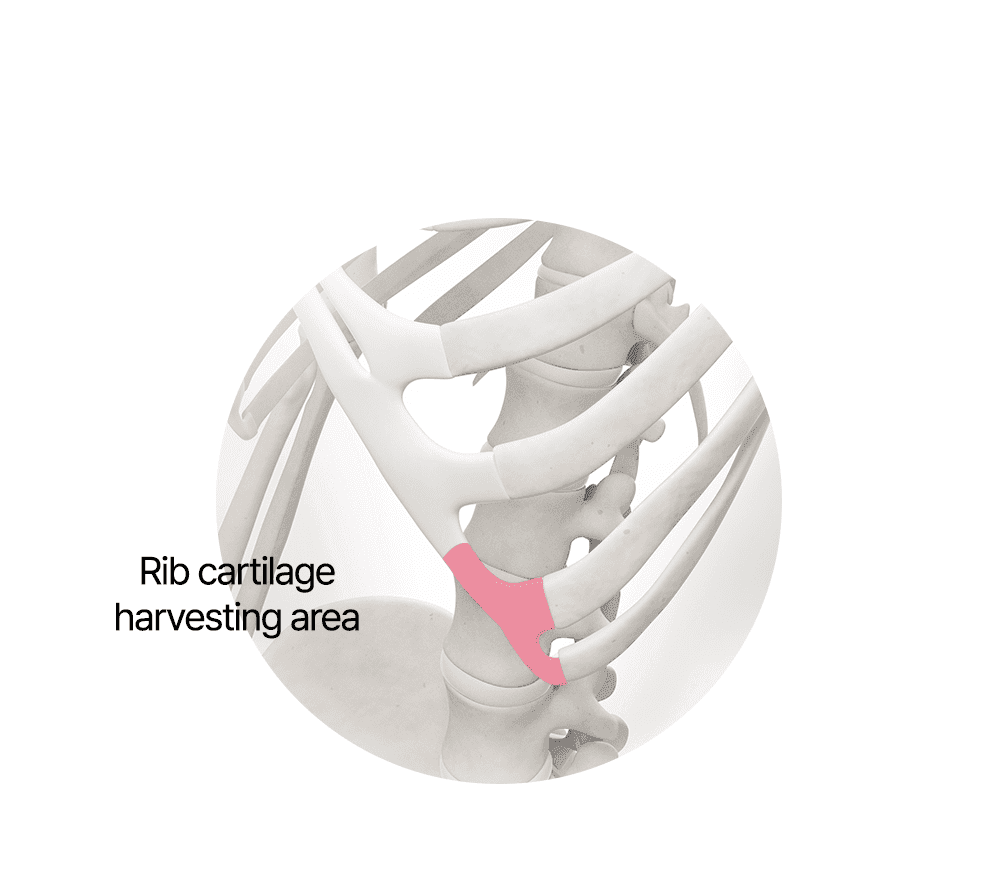
Correction Using Rib Cartilage
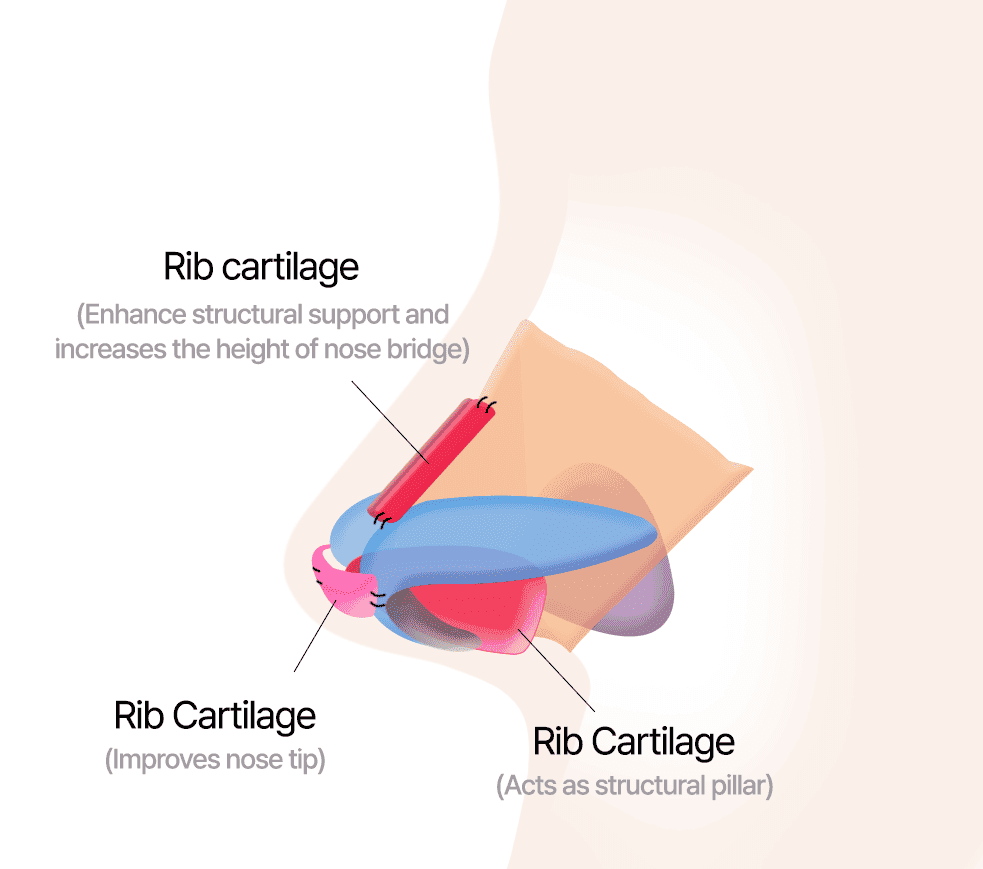
1. Septal Cartilage That Does Not Require an Additional Incision
Septal cartilage is located inside the nose, so no additional
external incision is required and can also address rhinitis symptoms.
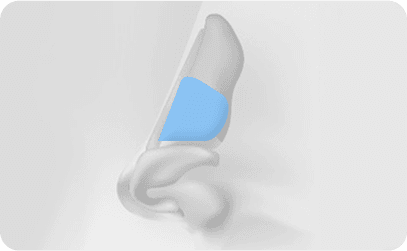
- Appropriate thickness and strength
- Allows nasal bridge augmentation or lengthening
- No additional incision required as it is harvested from inside the nose
2. Ear Cartilage With Excellent Flexibility and Elasticity
Ear cartilage has a rounded shape and flexible properties
properties similar to the natural nose and is highly
useful for shaping the nasal tip and compensating for
areas where septal cartilage is insufficient.

- Compensates for areas where septal cartilage is insufficient
- Accessed from behind the ear, leaving no visible scars
- Soft texture, suitable for natural nose tip
3. Autologous Rib Cartilage With Strong Durability and Support
Compared to septal or ear cartilage, rib cartilage can be
harvested in larger quantities. Its superior strength and
durability allow it to maintain nose tip over time without
collapse, making it a frequently used autologous material.
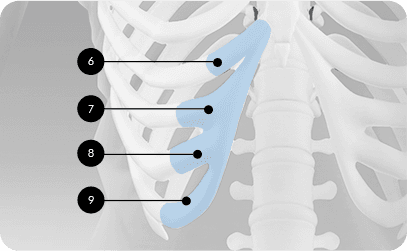
- Strong structural support helps prevent nasal tip drooping
- Cartilage from ribs 6-9 is custom-harvested and designed according to individual needs
- Largest harvest volume compared to septal or ear cartilage, allowing sufficient nose bridge lengthening
- Comprehensive scar care system for rib cartilage donor sites
AB's Strong Point
Why Choose AB for Implant-Free Rhinoplasty
1. Fast and Precise Autologous Tissue Harvesting with Minimized Warping
Minimized pain through careful dissection without muscle damage
Safe rib cartilage harvesting with an on-site anaesthesiologist
One-on-one customized rib cartilage harvesting (from ribs 6, 7, 8, or 9)
Precise carving and design to minimize warping, supported by extensive experience and advanced techniques
2. Naturally Defined Lines with Long-Lasting Results
CASE 1. Side View


CASE 2. 45° View


3. Advanced 3D-CT Precision Diagnosis
structure of the nasal septum
improves nasal function along with
aesthetic correction
conduct a systematic examination and establish
a precise surgical plan

4. Columella Shape and Angle That Best Complement the Facial Profile
There is no single fixed angle for the nasolabial area.
By considering overall facial length and proportions, we refine the nasal
angle to create a harmonious and well-balanced facial profile.
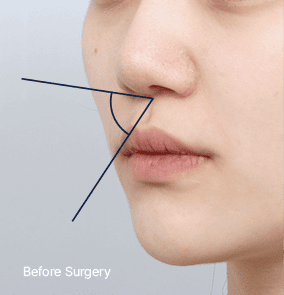

A recessed philtrum and
a flatter side profile
A balanced and harmonious profile with
improved nasal and philtral angles
#AB’s Personalizedd Diagnosis and Care System
From consultation to full recovery, we promise dedicated one-on-one care, with
the same medical team taking full responsibility throughout the entire process.
Comprehensive 1:1 Responsible Care Throughout the Entire Journey
1: 1 Personalized Consultation
Surgery Performed Directly by the Consulting Specialist
Close Monitoring by a Dedicated Anesthesiologist

Personalized Management by a Dedicated Consultant

Progress Monitoring and 1:1 Postoperative Care
Implant-free Rhinoplasty Surgery Information
INFORMATION SURGERY
Surgery Information
Surgery Duration
1 hour ~ 1 hour 30 min
Anesthesia method
Sedation
In-hospital Treatment
2~3 times
Recovery Period
After 7 days
RECOMMEND SURGERY
Recommended Candidates
Individuals with thin skin who are concerned about implant visibility
Individuals who worry about inflammation or side effects related to artificial implants
Individuals seeking a natural-looking nasal line
Individuals with concerns such as a flat nose or upturned nose
Loading...
Frequently Asked Questions about Rhinoplasty
It is generally recommended to start wearing glasses approximately one month after rhinoplasty.
If you were already wearing glasses before surgery, extra caution is required when wearing them after the procedure.
First, wearing glasses during the early postoperative period may cause pressure due to their weight, which can potentially shift the implant.
Second, even after rhinoplasty, the implanted material may not be fully stabilized, and wearing glasses during this stage may increase the risk of implant movement.
Typically, after about one month, the implant gradually adheres to the surrounding tissues and becomes more stable, significantly reducing the risk of movement.
Therefore, we advise patients to avoid wearing glasses for at least one month after surgery.Yes. Regardless of the severity, including a crooked nose, nasal correction is possible through rhinoplasty.
When patients visit for consultation, they often describe a “crooked nose” differently based on their own perspective.
In most cases, this refers to a nose that does not appear straight from the front where the nose bridge, from the glabella (between the eyebrows) to the nasal tip, deviates to one side around the mid-portion.
In some cases, patients may refer to a nose that appears uneven or irregular from the side such as a dorsal hump as a “crooked nose.”
Rhinoplasty can address a wide range of concerns, including crooked noses, hump noses, low bridges, short noses, and bulbous noses. Therefore, there is no need for excessive concern, as these conditions can be effectively corrected through appropriate surgical planning.If the area that was impacted is only mildly red, there is a high possibility that no fracture has occurred.
However, if you feel that the swelling at the impacted area is relatively severe, further evaluation may be necessary to determine whether a fracture has occurred.
When swelling is significant, it can be difficult to immediately assess the presence of a fracture. In such cases, we recommend continuing cold compresses on the affected area and visiting the surgical clinic approximately 1–2 weeks later for a CT scan and a thorough evaluation by the attending specialist.
Even if a fracture is identified, if there is no significant issue with the implant position or the nasal septum, most cases can be managed with observation alone without additional treatment.
Therefore, there is usually no need for excessive concern.Autologous dermis begins to undergo absorption from the moment it is transplanted. Therefore, unlike implants, it may be more difficult to achieve or maintain a clearly defined and predictable change.
Due to the inherent characteristics of autologous dermis, there are certain limitations during surgery. The most significant limitation is that postoperative outcomes are more difficult to predict compared to implant-based rhinoplasty.
In addition, unlike implant rhinoplasty which typically produces a sharp and well-defined nasal bridge where autologous dermis placed on the nasal bridge has a softer tissue quality and may feel similar to natural soft tissue when touched.
If a patient has a clear preference for a high, prominent, and well-defined nasal bridge and tip, autologous dermis rhinoplasty may not be the most suitable option.
However, in cases where a patient has undergone multiple revision surgeries resulting in thin nasal skin, or when there is a higher risk of complications, autologous dermis rhinoplasty may be more advantageous than implants.
Rather than deciding on an implant in advance, it is important to carefully assess the current condition of the nose and determine the most appropriate surgical method through a thorough consultation with a board-certified plastic surgeon.The most common reason for undergoing revision rhinoplasty is a condition known as capsular contracture.
Capsular contracture is a complication in which inflammation occurs due to issues with the implant placed during the initial rhinoplasty. This can cause the nasal skin to become firm, the nasal tip to retract, and the nose to appear shorter.
Since these changes are often visible externally, it is important to notify the original surgical clinic as soon as possible and undergo proper evaluation to identify the cause.
Although capsular contracture can be psychologically stressful, leaving it untreated may result in progressive nasal deformity. Therefore, revision surgery is required to remove the existing implant and replace it with a new one. During the procedure, any adhesions within the nasal tissue must be carefully released, making the surgery technically demanding.
If the concern is purely aesthetic—such as dissatisfaction with the postoperative shape—and there is no inflammation or functional issue, it is generally recommended to wait at least 6 months to 1 year for the nasal tissues to fully recover before considering revision surgery in order to achieve stable and reliable results.
Safety System
Through various safety management systems, patients can receive surgery with greater peace of mind.

On-site board-certified specialist in Anesthesiology and Pain Medicine
Anesthesiology and pain medicine specialists manage the entire surgical process from pre-operation through post-operation.

Real-time monitoring during anesthesia
Anesthesiologists monitor patients in real time during surgery, with dual and triple verification through central monitoring systems.

Pre-surgery safety check
For safer surgery, we conduct comprehensive pre-operative examinations through our in-house self-inspection system.

University hospital–level safety equipment
Through various safety management systems, patients can receive surgery with greater peace of mind.
Make your own plan for Korean Plastic Surgery
Please note that the actual medical schedule may vary depending on each patient's individual condition,
such as health status, and the specific surgical procedures involved.
Tailored to meet individual needs,
our service ensures that your medical tourism journey is planned
with the utmost care and precision, considering your unique medical requirements
Date of surgery
Eye Surgery
Nose Surgery
Fatgraft
Lifting
Accu
Breast Surgery
Body Shaping
liposuction
Lip
Facial Contouring
Skincare
Stem Cells
| SUN | MON | TUE | WEN | THU | FRI | SAT |

- WeekdayAM 10:00 ~ PM 7:00
- SaturdayAM 10:00 ~ PM 5:00
- Evening HoursAM 10:00 ~ PM 09:00 (Fri)
*Closed on Sundays and Public Holidays



